Sep 19, 2019 by spinalcare
Heat vs. Ice Crash Course
Have you ever been confused when to choose heat and when to choose ice for your injury? You are not alone, here at Spinal Care we get that question almost daily. We are here to clear up the confusion!
Both heat and ice work to relieve pain but only when used at the appropriate time…. So here is your heat and ice crash course!
Let’s start with what how they each work…
- Heat: Heat relaxes muscles and softens tissues increasing joint/muscle range of motion. Heat therapy causes an increase in local blood flow resulting in an increase in the amount of oxygen and nutrients to the applied area. Heat packs also confuse sensory nerves decreasing your perception of pain.
- Ice: Cold therapy slows circulation thus decreasing blood flow to the area resulting in a reduced swelling and inflammation. Reduced inflammation results in a reduction of inflammatory markers (ie. Histamine) which are pain provoking!
When should I use them?…
- Heat: Use heat therapy on injuries after inflammation has subsided, general rule is use after the first 48-72 hours post-injury. Heat therapy is safe to use on chronic aches from joint pain, arthritis, muscle spasms and sore muscles to help stimulate blood flow. Heat is generally best for more chronic issues.
- Ice: Use ice therapy on injuries that have occurred in the last 24 hrs. A general rule is to think ice when areas are swollen, warm to touch, inflamed or bruised. Using ice immediately after an injury can help control the inflammatory response early on (if left uncontrolled inflammation can lead to pain, swelling, decreased range of motion and decreased strength).
How long should I apply?…
- Heat: Maximum application is 20-30 minutes to reach full vasodilation.
- Ice: 10-15 minute sessions with a covered ice pack (dish towel/paper towel), never exceed 20 minutes to prevent frostbite.
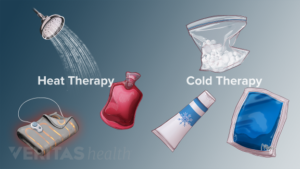
Remember to take caution – key facts to keep in mind.
- Heat: Do not apply heat to an area that is inflamed as this may lead to increased swelling and a prolonged recovery. Do not leave a heating pad or device on for too long as burning may occur. Heating for longer than 20-30 minutes can cause a rebound effect which may result in constriction of the blood vessels leading to more pain.
- Ice: If you are looking for relief of stiff/tight muscles cold therapy may prevent them from loosening causing more pain. With ice therapy it is important that sessions last no longer than 10-15 minutes as ice therapy that is too long may lead to frostbite. Be sure use a cloth or towel to protect to skin from direct application of ice.
- Other contraindications of heat or ice therapy: Avoid areas of impaired circulation (often in diabetic patients), areas with no sensation to heat or cold, any area with the presence of a skin infection, severe cardiac disease, hemorrhagic tendencies.
Contrast therapy…
- Contrast therapy involves the alternation of ice and heat therapies for short durations. Contrast therapy is gentle and controls inflammation while simultaneously increasing circulation resulting in the best of both worlds. Generally, acute sprain/strain injuries, joint aches, chronic pains respond best to contrast therapy.
What should you do after your visit to Spinal Care?
- The treatment you receive at Spinal Care often results in a temporary increase in inflammation before the body starts to heal. We recommend icing after your visit as it will reduce the inflammation and pain. Many patients find that they don’t need to ice but you definitely do not want to apply heat to any area we have worked.
If you have any questions please contact your friends at Spinal Care, we would be glad to help you understand further!
References:
“ACSM’s Primary Care Sports Medicine” Mckeag, D. B., & Moeller, J., L. (2nd edition, 2007).
“Differential Diagnosis and Management for the Chiropractor” Souza, T, A. (5th edition; 2016).
